What is the story on Donald Trump’s hair? He looks like he is trying to hide something?
 As I understand it, Donald Trump was a victim of the old hair transplant process starting in the 1980s. The quality of the work most probably resulted in the pluggy look, and he possibly had scalp reductions (which were popular in those days). Between the two, he might have little donor hair left. There may be significant scarring as well if he had many procedures in the ‘old days’. He apparently found the solution to cover up his hair loss problem, with a creative hair styling that he is now well known for. He knows that his hair is the subject of much focus and with people who just love to talk or make their living hosting entertainment shows. That is the price of today’s celebrity.
As I understand it, Donald Trump was a victim of the old hair transplant process starting in the 1980s. The quality of the work most probably resulted in the pluggy look, and he possibly had scalp reductions (which were popular in those days). Between the two, he might have little donor hair left. There may be significant scarring as well if he had many procedures in the ‘old days’. He apparently found the solution to cover up his hair loss problem, with a creative hair styling that he is now well known for. He knows that his hair is the subject of much focus and with people who just love to talk or make their living hosting entertainment shows. That is the price of today’s celebrity.
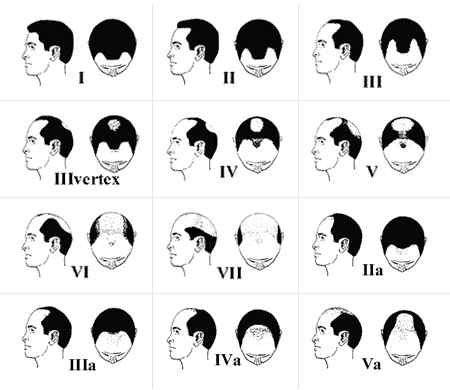
What he has done is to exploit a ‘comb-forward’ style, maximizing what hair he has to cover what he wants to hide. Like the comb-over, it layers hair from one part of the scalp to another (comb-forward means that the hair is kept long and combed to the front). I call this the ‘Trump style comb-forward’ in my private office practice, because of his celebrity status. This style uses what many people with frontal balding exploit (see the Norwood Class 3 or 4 pattern balding). The less hair that is lost and the more hair that remains, the more effective is the result of styling to hide thinning or balding in the frontal area. When taken to extreme, whether it is the comb-over or the comb-forward, the appearance does not look good.
When any reasonable amount of hair is transplanted in the Class 3 or 4 balding pattern (those with natural Norwood Class frontal balding patterns), a comb-forward can work even better so restoring all of the missing density is not needed. Nobody ever knew that CBS News sports reporter Steve Hartman was balding and he perfected the combing to the front and side enough to hide his thinning hairline. This canopy comb-forward was very effective for him (a common combing style for many men), but he was slowly losing the battle to preserve his look. Many men tell me that they spend more and more time dealing with their hair, not only in the mornings, but throughout the day as well. One man who comes to mind told me that his comb was like his Mont-blanc pen, always needed wherever he went and he carried hair spray with him to touch up the styling in bathroom breaks that he had to take quite often. Steve’s hair, on the other hand, was very cooperative with a strong character that easily laid down the way he wanted it to. Rather than waiting too long and risking an unnatural appearance, Steve decided to take the bull by the horns and had one transplant procedure (see pictures). Steve went for natural fullness as he did not want to maintain any illusion at all, so we put as much hair as we could safely move in just one transplant session. The point between where Steve came from and a really bad comb-over (the kind that everyone sees on TV or at the airport), is a slow, insidious process — so slow in fact, that the person who is doing it never notices the advancing balding nor the progressive failure of the grooming style. I always wonder why family members do not comment on the failure of this styling process, but maybe they are just not saying anything early enough and now are embarrassed to say anything at all so late in the process.
Some men with bad comb-overs deny their evolving look, putting a mental block on the unnatural appearance they evolved, and others just stop going out into the public arena. Hats and wigs solve the problem for some, a type of cover-up that does not work for everyone and I have seen a few take it to extreme levels, creating a bouffant style with hair that is one or two feet long and combed into a circlular pattern, layered hair by hair to mimic what the person thinks is normal.
I have been asked many times why the rich and famous who can afford the best doctors don’t just get the best surgical hair restoration money can buy. Ignorance is part of the answer. I believe that many men with the old deforming hair transplants find themselves in a difficult situation. They may not know that they were going down that road when the process initially started. When they found out, they may have come to the conclusion that it was too late to do something about it. With luck, men in this predicament may find some solution that they learn to live with when it works (comb overs, hats, wigs, scalp coloring agents, and the like) or they may find their way to a good hair transplant surgeon who can fix the problem.
With today’s modern Follicular Unit Transplant and Follicular Unit Extraction (FUE) techniques, some amazing work can be done. With FUE in particular, it is virtually for all practical purposes scar-less and the procedure is minimally invasive. Not everyone can be brought back to “normal” if too much of the hair has been squandered, or if scarring has gone too far. If Mr. Trump had old type plugs, he can have that hair redistributed so that the big bad plugs are no longer present. Any hair that is moved can be put to better esthetic use in other scalp locations under the guidance of an artistic hair restoration surgeon (see Dean’s Story for an example of this).
Had Mr. Trump been a patient of ours, I could never have written anything about him because patient privacy is central to the way doctors operate their business today. I hope that by writing this piece in answer to your question, I have not offended him in any way.

 Wigs, when worn by men, can look great at times, but if you’ve ever spotted someone wearing a wig, you know that they also can stand out as pretty bad (the old rug on a head look). Good hair systems are costly (possibly thousands of dollars a year). They require constant maintenance and they do wear out. Everyone having them must have at least two of them, each often costing over $2,000 and those that are made for the ‘upper class wealthy people’ are significantly more, I am sure. The hair grows under the wig, so these wigs must be removed and repositioned with fresh glue after the scalp is shaved. Eventually, the glues used will produce traction hair loss so that all of the hair in the glued areas will be lost. As many as two or three maintenances per month are often required and that costs $$$ if you have your special stylist folks do it for you, pushing up the annual costs substantially. To avoid odor from developing, the wig and the scalp must be washed regularly. Can you imagine wearing a T-shirt day after day and what it might smell like after just a few days? This is a characteristic odor that reflect body oils in decay. The scalp is no different, as it sheds skin at a high rate which also undergoes decay, so it must be scrubbed off with frequent washings, taking off the hair system and replacing it regularly. Many men with hair systems are tense when in intimate situations, as they have a no touch zone around their head. Can you imagine a woman running her fingers through your hair and have the piece come off in her hand, or her finger nails catch on it. No way! So men with hair systems do not allow intimacy to go as far as to let a woman touch their hair.
Wigs, when worn by men, can look great at times, but if you’ve ever spotted someone wearing a wig, you know that they also can stand out as pretty bad (the old rug on a head look). Good hair systems are costly (possibly thousands of dollars a year). They require constant maintenance and they do wear out. Everyone having them must have at least two of them, each often costing over $2,000 and those that are made for the ‘upper class wealthy people’ are significantly more, I am sure. The hair grows under the wig, so these wigs must be removed and repositioned with fresh glue after the scalp is shaved. Eventually, the glues used will produce traction hair loss so that all of the hair in the glued areas will be lost. As many as two or three maintenances per month are often required and that costs $$$ if you have your special stylist folks do it for you, pushing up the annual costs substantially. To avoid odor from developing, the wig and the scalp must be washed regularly. Can you imagine wearing a T-shirt day after day and what it might smell like after just a few days? This is a characteristic odor that reflect body oils in decay. The scalp is no different, as it sheds skin at a high rate which also undergoes decay, so it must be scrubbed off with frequent washings, taking off the hair system and replacing it regularly. Many men with hair systems are tense when in intimate situations, as they have a no touch zone around their head. Can you imagine a woman running her fingers through your hair and have the piece come off in her hand, or her finger nails catch on it. No way! So men with hair systems do not allow intimacy to go as far as to let a woman touch their hair. I have followed Bruce Willis’ hair loss over the years from his thinning during the TV series
I have followed Bruce Willis’ hair loss over the years from his thinning during the TV series  Now I’m not a huge sports nut, but I read enough news to know what’s going on. The nation seems to be obsessed with the hair, or lack thereof, of the Seattle Seahawk’s quarterback Matt Hasselbeck. I caught a few sportscasters on ESPN talking about his “shiny dome†a few nights ago, and since, I have noticed numerous respected sports journalists harping on, or even supporting, Matt Hasselbeck because he is bald.
Now I’m not a huge sports nut, but I read enough news to know what’s going on. The nation seems to be obsessed with the hair, or lack thereof, of the Seattle Seahawk’s quarterback Matt Hasselbeck. I caught a few sportscasters on ESPN talking about his “shiny dome†a few nights ago, and since, I have noticed numerous respected sports journalists harping on, or even supporting, Matt Hasselbeck because he is bald.